Effect of Ubiquinol Therapy on Sperm Parameters and Serum Testosterone Levels in Oligoasthenozoospermic Infertile Men
1 Professor & Head, Department of Biochemistry, GMCJagdalpur(C.G), India.
2 Professor, Department of Biochemistry, Biology and Genetics, Polytechnique University of the Marche, Ancone, Italy.
3 Director, Research, Kaneka Corporation Ltd., Japan.
4 Dean & Professor, Department of Medicine, Government Medical College, Jagdalpur(CG), India.
5 Associate Professor, Department of Biochemistry, GMC(CG), India.
6 Associate Professor, Department of Gynecology, GMC(CG), India.
NAME, ADDRESS, E-MAIL ID OF THE CORRESPONDING AUTHOR: Dr. Amar Singh Thakur, Professor and Head, Department of Biochemistry, LtBRKMGovt. Medical College, Jagdalpur, Chhattisgarh– 494001, India. E-mail : drasthakur2004@yahoo.co.in
Introduction
The male sperm counts decline due to environmental factors, such as pesticides, heavy metals and exogenous estrogens causing negative impact on spermatogenesis. The low testosterone levels are associated with lower levels of antioxidants that protect against free radical damage to glands that produce testosterone. The earlier studies showed that the supplementation of vitamins and antioxidants including 10mg Ubiquinol per-day increases in sperm count and motility.
Materials and Methods
The Ubiquinol is strong antioxidant, hence in view of the above study 150 mg/day Ubiquinol was supplemented to 60 men with age group of 20-40 years. The patients were supplemented for six months, the testosterone level and sperm parameters were analysed before and after supplementation of Ubiquinol every month up to six months. The total sperm count increased by 53% (p<0.05).
Results
The total sperm motility was observed 26% (p<0.05) high after supplementations. Out of total motility, the quantity of rapidly motile sperm increased 41% (p<0.05). The number of sluggish motile sperm was decreased approximate 29% (p<0.05). The non motile sperm count was also decreased up to 55% (p<0.05).
Conclusion
The testosterone level is maintained during the study and morphology of flagella of sperm has improved. The finding suggests that the supplementation of Ubiquinol may be beneficial for oligospermic patients.
Amar Singh Thakur, Gian Paolo Littarru, Iwao Funahashi, Umeshwar Singh Painkara, Narendra Shriram Dange, Prabha Chauhan, .EFFECT OF UBIQUINOL THERAPY ON SPERM PARAMETERS AND SERUM TESTOSTERONE LEVELS IN OLIGOASTHENOZOOSPERMIC INFERTILE MEN.Journal of Clinical and Diagnostic Research [serial online]2015 Sep[cited:2016 Mar 1] 9 BC01 – BC03
Available from
http://www.jcdr.net//back_issues.asp
Ubiquinol is a vitamin-like substance found in body cells, especially in the heart, kidney, liver and pancreas that may promote health by fighting against cardiovascular diseases, hypertension, diabetes mellitus and infertility, etc. Scientists believe Ubiquinol functions as an antioxidant that blocks actions that can damage cells. Decreased sperm motility is one of the leading causes of male infertility [1]. One of the rational strategies to counteract the oxidative stress in seminal plasma is to increase the antioxidant level [2].
The induction of different concentrations of ubiquinol with different medical or surgical procedures in male infertile patients is used to identify its physiological role. The Ubiquinol concentration and distribution between seminal plasma and spermatozoa in varicocele, before and after surgical treatment and in infertile patients have been evaluated to observe its physiological role [1].
The environmental risk factors responsible for deteriorating sperm quality are heat, radiation, exposure of environmental estrogens, pesticides, cigarette smoking, alcohol consumption, chronic stress, nutritional deficiencies. Another environmental concern with infertility is the toxic effects of heavy metals on sperm quantity and production. The prevalence of heavy metals like lead and its potentially negative interactions with the neuroendocirne system has been shown to cause male infertility [3].
Human spermatozoa has a capacity to generate Reactive Oxygen Species (ROS) in all its cell types, such as superoxide anion (O2-), hydroxyl radical (.OH), hydrogen peroxide (H2O2) and the hypochlorite radical (.OHCL) under aerobic conditions. Superoxide anions (.O2-) are generated as primary product of ROS which is further converted into hydrogen peroxide (H2O2) the intracellular superoxide dismutase (SOD) enzyme. The nitrogen derived free radical nitric oxide (NO.) which is also an important mediator for normal cell function causes damage in addition to ROS [4].
The sperm physiological processes, such as capacitation, hyperactivation and sperm oocyte fusion are actively mediated by free radicals (ROS). The polyunsaturated fatty acids (PUFA)
of the sperm plasma membranes are vulnerable to attack by ROS, these ROS trigger a chain of chemical reaction known as lipid peroxidation of sperm membrane polyunsaturated fatty acids [5].
Under normal circumstances the production and concentration of ROS is balanced by the antioxidant scavenging systems. The sperm loses its integrity due to peroxidative damage of sperm plasma membrane by seminal oxidative stress of male reproductive tract & moreover spermatozoa are sensitive to oxidative stress (OS) because they lack cytoplasmic defenses [6].
The retention of the excess residual cytoplasm (cytoplasmic droplets) causes production of ROS which leads to synthesis of H2O2 in morphologically abnormal spermatozoa and in immature spermatozoa. The free radicals like H2O2 which can cross the sperm cell membrane inhibits the enzyme activity such as Glucose -6-Phosphate dehydrogenase (G6PDH) due to which a deficiency of NADPH & concomitant accumulation of oxidized glutathione & reduced glutathione occurs. These changes decrease antioxidant defense system of spermatozoa which ultimately leads to the membrane lipid peroxidation [2].
Most of the earlier studies [7–11] have failed to examine the effect of antioxidants on a specific group of infertile patients with high oxidative stress. The benefit of antioxidants as a treatment modality for patients with male infertility requires study with statistically acceptable sample size to reach evidence based conclusion [2].
In infertile men with idiopathic asthenzoospermia (the loss or reduction of sperm motility in semen), physicians may want to add ubiquinol in their treatment modality [12].
The sperm production and its functions are highly energy dependent processes. Ubiquinol deficiency could presumably be a contributing factor of infertility in men [13]. Further studies are required to determine whether Ubiquinol therapy has a role in the treatment of infertility.
This study has been undertaken due to prevalence of male infertility cases in this region as per hospital records. Also the soil of Bastar region (main source of drinking water for local tribals) contains minerals and heavy metals with prolonged exposure of which interferes normal sperm function [3]. The aim of the study was to analyse the complete sperm parameters of villagers having oligospermia, reporting to hospital outdoor patient department (OPD). The parameters evaluated were: Sperm count, Motility, Physical characteristics and measurement of testosterone level to analyse the testicular cells response to Ubiquinol.
Sixty male patients, of age group between 20-40 years, who were not under any treatment for oligospermia were included in this study.
The sample selection was done by analysing the semen samples by physician and gynecologist. Patients who were facing difficulties in conceiving even after completion of two years of marriage were selected for this study, with no history of diabetes, obesity, thyroid disorders, alcoholism, chewing of tobacco, cigarette smoking. Patients with oligospermia or any other clinical manifestations were included in this study.
The study period was two years (from Jan-2013 to Jan-2015) and the follow up of the patients within the period with ubiquinol supplementation was 6 months. The dose was 150mg of Ubiquinol (as most of the studies with duration of 24-26 weeks [1,14] have been done with 150-200 mg dose per day), in the form of capsule as prescribed by the physician and gynecologist. The complete course of medicine (150 mg of ubiquinol) were provided by the researches to all the oligospermic patients.
The study parameters were estimated by standard techniques prescribed by world health organization [15] before supplementation, under supplementation (after every 2 months) and after complete supplementation upto 6 months.
After counseling the patients and taking their consent, the sample collection was done by using all aseptic precautions.
The testosterone level was measured by ELISA method [14]
Statistical analysis was performed using the paired two sample t-test. Results are reported as Mean±S.D. Differences among the samples were evaluated by student t-test. Variance and pearson correlation were analysed among variables.
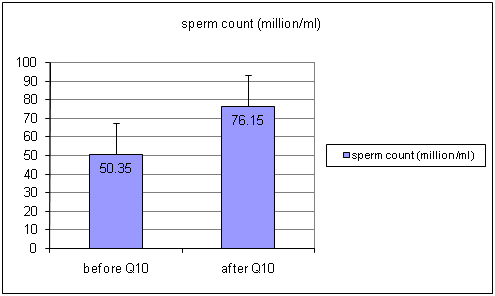
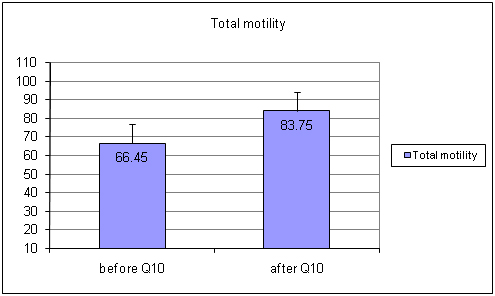
The results showed, the total sperm count increased by 53% (p<0.05) [Table/Fig-1] (Before Ubiquinol 50.35±33.2 and after Ubiquinol 76.15±39.81) and the total sperm motility was observed 26% high (p<0.05) [Table/Fig-2] (before Ubiquinol 66.45±21.34 After Ubiquinol 83.75±14.04) after Ubiquinol supplementations.
Showing graph of sperm count levels before and after treatment
Showing graph of total motility levels before and after treatment
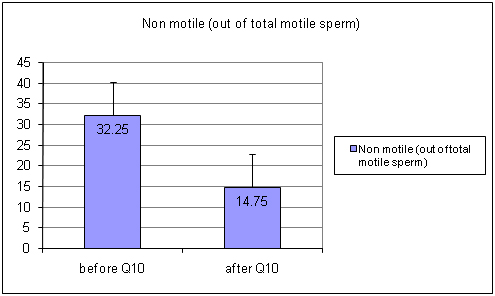
 Out of total motility, the quantity of rapidly motile sperm increased upto 41 % (p<0.05) [Table/Fig-3] (before Ubiquinol 42.5±24.8 after Ubiquinol 59.8±23.79) and the number of sluggish motile sperm was decreased approximately 29% (p<0.05) [Table/Fig-4] (Before Ubiquinol 56.5±24.66 After Ubiquinol 40.2±24.01). The non motile sperm count was also decreased up to 55% (p<0.05) [Table/Fig-5] (Before Ubiquinol 32.25±20.93, After Ubiquinol 14.75±14.09). The testosterone level was maintained within the normal range during the study [Table/Fig-6] (before Ubiquinol 3.865±1.154; After Ubiquinol 4.0±1.42).
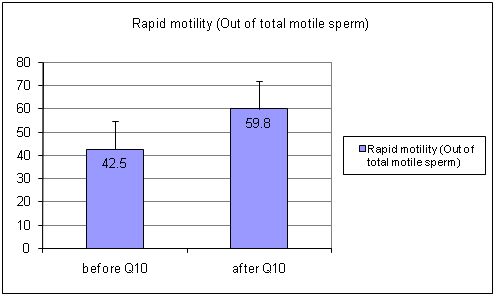
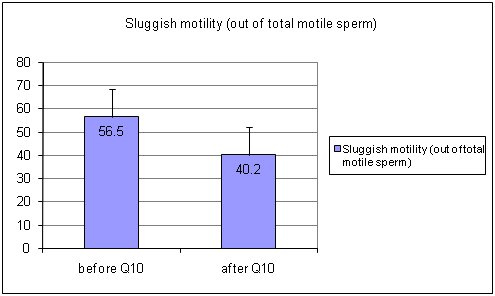
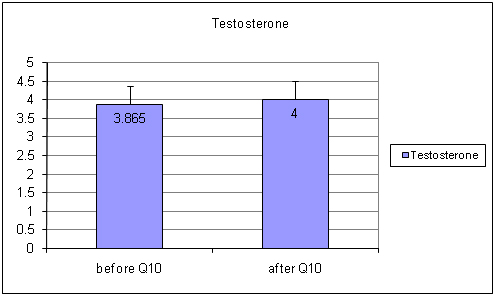
Out of total motility, the quantity of rapidly motile sperm increased upto 41 % (p<0.05) [Table/Fig-3] (before Ubiquinol 42.5±24.8 after Ubiquinol 59.8±23.79) and the number of sluggish motile sperm was decreased approximately 29% (p<0.05) [Table/Fig-4] (Before Ubiquinol 56.5±24.66 After Ubiquinol 40.2±24.01). The non motile sperm count was also decreased up to 55% (p<0.05) [Table/Fig-5] (Before Ubiquinol 32.25±20.93, After Ubiquinol 14.75±14.09). The testosterone level was maintained within the normal range during the study [Table/Fig-6] (before Ubiquinol 3.865±1.154; After Ubiquinol 4.0±1.42).
Showing graph of rapid motility levels before and after treatment
Showing graph of sluggish motility levels before and after treatment
Showing graph of non motile levels before and after treatment
Showing graph of testosterone levels before and after treatment
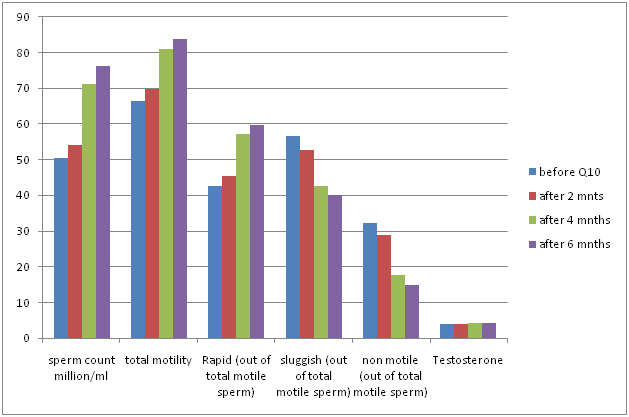
Showing comparitive graph of sperm parameter levels before and after treatment
A 2004 study in the Journal Fertility and Sterility looked at the effects of a 200 mg daily Ubiquinol supplement on the sperm counts of 22 infertile men with low sperm motility. Before the start of the study, the infertile men had lower than average levels of the Ubiquinol in the seminal fluid. After six months of taking the supplement, the men showed increased levels on Ubiquinol. The research also found that the men’s sperm motility increased as well [1].
“The exogenous administration of CoQ [10] increases both ubiquinone and ubiquinol levels in the semen and can be effective in improving sperm kinetic features in patients effected by idiopathic asthenozoospermia, due to its involvement in mitochondrial bioenergetics and its antioxidant properties” [1,12].
Earlier studies have proved that semen parameters were statistically improved with the supplementation of Ubiquinol. However, further studies are needed to draw a final conclusion on the effect of Ubiquinol supplementation on the pregnancy rate [16].
Ubiquinone inhibits lipid peroxidation by preventing the production of lipid peroxy radicals, reduces the initial perferryl radical and singlet oxygen and also regenerates other antioxidant such as vitamin E [17,18].
A study showed that, Ubiquinol group had a significant decrease in serum follicle-stimulation hormone and luteinizing hormone at the 26-week treatment phase. The investigators highlight that a lower serum follicle-stimulation hormone implies better spermatogenesis [19].
The result suggests that supplementation of Ubiquinol helps in increasing the sperm count along its motility.
The testicular cells secretes a normal level of testosterone may be due to reduced oxidative damage in presence of lipophilic antioxidant ubiquinol. The flagella having long exposed structure is more prone to oxidative damage. The presence of ubiquinol might have reduced the oxidative stress and prevented the oxidative damage to the flagella structure, which helps in sperm motility, thus by maintaining the size of flagella which helps in increasing the sperm motility [4].
Hence, the Ubiquinol therapy may be useful for the treatment of male infertility as it has significant effect on sperm parameters.
The study concludes that supplementation of 150 mg of Ubiquinol is beneficial for oligospermic patients, further study is required with large number of patients by increasing the doses of ubiquinol to see the beneficial effect and to draw more significant statistical data.
[1]. Balercia G, Mancini A, Paggi F, Tiano L, Pontecorvi A, Boscaro M, Coenzyme Q 10 & male infertility J Endcrinol Invest 2009 32(7):626-32.
[2]. Afarwal A, Saleh RA, Role of oxidants in male infertility: rationale, significance and treatment Urol clin N Am 2002 29:817-27.
[3]. Sindair S, Male infertility: Nutritionla and environmental considerations Altern Med Rev 2000 5(1):28-38.
[4]. Sharma RK, Role of reactive oxyen species in male infertility (Clinical review). From the Andrology Research & Clinical laboratories, Dept. of Urology, The Cleveland foundation, Cleveland Ohio. Urology 1996 48(6):835-50.
[5]. Agarwal A, Sushil A, Prevention of Oxidative Stress Injury to Sperm Journal of Andrology 2005 26(6):654-60.
[6]. Agarwal A, Sekhon LH, The role of antioxidant therapy in the treatment of male infertility Human Fertility 2010 13(4):217-25.
[7]. Martin-Du Pan RC, Sakkas D, Are antioxidants useful in the treatment of male infertility? Hum Reprod 1998 13:2984-85.
[8]. Suleiman SA, Ali ME, Zaki ZMS, Lipid peroxidation and human sperm motility: protective role of vitamin E J Androl 1996 17:530-37.
[9]. Abel BJ, Carswell G, Elton R, Randomized trial of clomiphene citrate treatment and vitamin C for male infertility Br J Urol 1982 54:780-84.
[10]. Moilanen J, Hovatta O, Excretion of alpha-tocopherol into human seminal plasma after oral administration Andrologia 1995 27:133-36.
[11]. Comhaire FH, Christophe AB, Zalata AA, The effects of combined conventional treatment, oral antioxidants and essential fatty acids on sperm biology in subfertile men Prostaglandins Leukot Essent Fatty Acids 2000 63:159-65.
[12]. Balericia G, Mosca F, Boscara M, Mancini A, Ricciardo-lamonica G, Littarru G, Coenzyme Q (10) supllementation in infertile men with idiopathic asthenozoospermia: an open, uncontrolled pilot study Fertil Steril 2004 81(1):93-98.
[13]. Gaby AR, The role of coenzyme Q 10 in clinical medicine. Part II. Cardiovascular disease, hypertension, Diabetes Mellitus and infertility Alternative Medicine review 1996 1(3):168-75.
[14]. Tietz NW, Text book of Clinical Guide to Laboratory Tests 1995 Third EditionPhiladelphiaW.B. Saunders Company:578-580.
[15]. WHO. Laboratory manual for the examination and processing of human semen. 5th edition: chapter-2; pp. 10 -102. ISBN: 978 92 4 154778 9
[16]. Safarinejad MR, Efficiency of coenzyme Q 10 on semen parameters, sperm function and reproductive hormones in infertile men The Journal of Urology 2009 182:237-48.
[17]. Schachter MB, 1996. Available from. http://www.mbschachter.com/coenzyme q10.htm
[18]. Thakur AS, Littaru GP, Moesgaard S, Dan Sindberg C, Khan Y, Singh CM, Hematological parameters and RBC TBARS level of Q 10 supllemented tribal sickle cell patients: A hospital based study Ind J Clin Biochem 2012 :1-4.doi:10.1007/s12291-012-0277-79
[19]. Littarru GP, Tiano L, Clinical aspects of coenzyme Q 10: An update Nutrition 2010 26:250-54.
